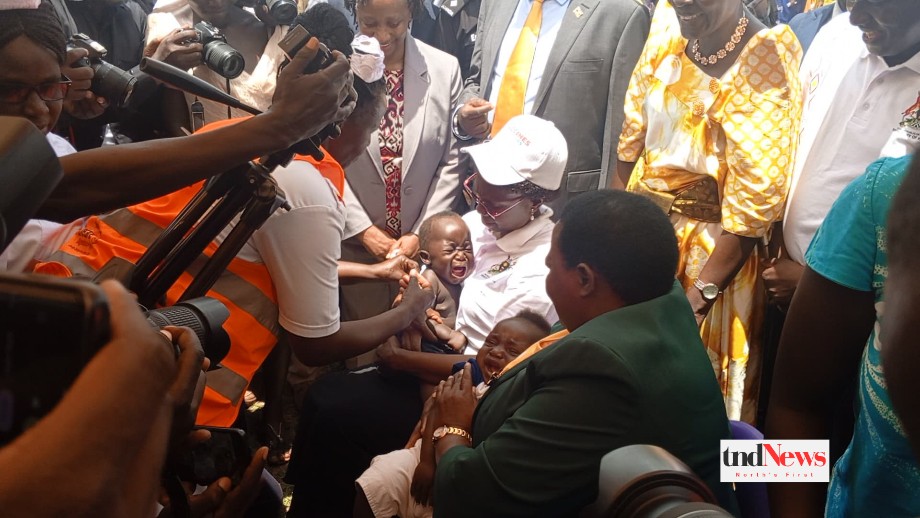Apac | The malaria vaccine was formally added to Uganda’s regular immunization schedule on April 2 by the Ministry of Health.
The event was hosted by the Apac municipality in East Lango, and Prime Minister Robinah Nabbanja was the chief guest. The vaccine’s introduction marks a historic step toward combating the deadly malaria disease that continues to afflict Uganda, particularly young children.
Malaria remains one of Uganda’s most serious public health issues, putting a significant strain on the country’s health system, economy, and society. It is the leading cause of illness and death in Uganda, and young children under the age of five are especially vulnerable.
According to the 2024 Health Management Information System (HMIS) report, approximately 32,900 people contract malaria daily in Uganda, causing significant disruptions in education and productivity.
Malaria claims the lives of sixteen (16) people every day, with children under five making up the majority of those killed.
In 2023 alone, Uganda recorded 12.6 million malaria cases, accounting for nearly 29% of the population affected by the disease.
This places Uganda among the top three countries in terms of malaria burden, accounting for 4.8% of all malaria cases worldwide. Despite numerous interventions, malaria remains a formidable challenge, highlighting the critical need for novel solutions.
Introduction of the malaria vaccine
The April 2, 2025 launch will include a comprehensive malaria vaccination campaign aimed at immunizing 1.1 million children, particularly those under the age of two.
The R21/Matrix-M injectable vaccine has proven to be an effective tool for reducing the malaria burden and preventing severe cases. To ensure maximum protection, the vaccine will be administered in four doses at ages 6, 7, 8, and 18 months old.
Prime Minister Robinah Nabbanja, who represented President Yoweri Museveni at the event, emphasized the historic nature of the malaria vaccine rollout.
“It is a bold step toward liberating our nation from the heavy burden of malaria, a disease that has for too long robbed our children of their futures, strained our health system, and hindered our socio-economic progress,” Nabbanja stated.
During the event, she also read a speech on behalf of President Museveni, who expressed his strong commitment to the fight against malaria and highlighted the government’s dedication to ensuring the health and well-being of the nation’s children.
The vaccination campaign will target districts with high to moderate malaria transmission rates, covering 105 out of Uganda’s 146 districts.
The government’s partnership with global organizations such as WHO, UNICEF, GAVI, and PATH will make the malaria vaccine available free of charge to eligible children, significantly enhancing access to this life-saving intervention.
In her remarks, Minister of Health Dr. Jane Ruth Aceng emphasized the pressing need to tackle malaria, highlighting the alarming statistics that demonstrate the continued burden of the disease in Uganda.
She described the introduction of the malaria vaccine as “a landmark achievement for the country,” emphasizing the importance of vaccination in reducing malaria severity and preventing complications such as cerebral malaria, severe anemia, organ failure, and death.
“In 2024 alone, Uganda recorded 10.9 million cases of malaria, with 3,582 deaths. This translates to 16 people dying every day, with 10 of them being children under the age of five. These figures are not just numbers; they represent families and communities suffering from a preventable disease,” Dr Aceng said.
Dr. Aceng pointed out that Apac district, where the vaccine launch was held, is particularly affected by malaria.
“Apac has been described as a ‘brigade of mosquitoes’,” she noted. “Last year, Apac recorded 41 deaths from malaria, including four children who died in just one month, which is a significant number compared to the national average.”
The Minister provided a detailed breakdown of APAC’s malaria burden, noting that “the test positivity rate stands at 66%, which is far higher than the national average of 42%.”
Additionally, the district has the highest infective bites, with 1,500 per person per year, which is equivalent to three infective bites per night.
Dr. Aceng also highlighted the concerning prevalence of malaria among pregnant women in the region. “In Apac, 74% of pregnant mothers tested positive for malaria, compared to the national average of 30%. In 2020, 3,801 pregnant women tested positive for malaria, and in 2024, that number rose to 4434,” she said.
“The statistics are clear: the malaria burden remains significant, and we must take urgent and coordinated action to combat this disease if we are to eliminate it from Uganda.”
She also underscored the critical role that malaria plays in Uganda’s healthcare system. “Malaria continues to be the leading cause of outpatient visits, accounting for 20% of hospital admissions and 10% of all deaths.”
The Minister, who also serves as Lira City woman MP, expressed her appreciation for the government’s partnership with GAVI, the Vaccine Alliance, in co-funding the purchase of malaria vaccine doses.
“This vaccine is a vital tool in the fight against malaria, and I am grateful for the support that has made this initiative possible.”
On a positive note, Dr. Aceng also took the opportunity to highlight Uganda’s progress in immunization. “Uganda now has 14 vaccines in our routine immunization schedule, up from just six in 1963. This progress is a testament to our commitment to improving child health.”
She also emphasized that the benefits of vaccines extend beyond the prevention of childhood diseases.

“Vaccines not only protect children from life-threatening diseases, but they also contribute to strengthening their ability to fight infections, reducing the financial burden on families, and enhancing school enrollment and retention. Additionally, we have seen a reduction in fertility rates to 5.2% as more women see their children surviving and thriving,” Aceng explained
The Minister concluded by noting the impact on infant mortality, which has decreased to 36 per 1,000 live births, signals a positive trend in Uganda’s overall health outcomes.
“We are taking a significant step forward in improving the health of our children and ensuring a brighter future for Uganda but the journey is far from over. Together, we must continue to fight malaria and work toward eliminating it in Uganda,” Dr. Aceng said.
She urged all parents and caregivers to ensure their children complete the four-dose vaccination regimen. “For optimal protection, the vaccine must be administered at 6, 7, 8, and 18 months. I encourage all parents to take full advantage of this opportunity.”
Local stakeholders weigh in
The malaria vaccination campaign has garnered widespread support from local health and government leaders.
Muwonge M. Abdulnoor, Chief Administrative Office (CAO) of Apac noted that the people in the district are no strangers to the heavy burden of malaria.
“I have always described Apac as a ‘mosquito base’ because of the overwhelming presence of this disease in our community. The malaria situation here is dire, and it’s high time we intensify our efforts.
“One of the most important strategies we can employ is more widespread spraying to reduce the mosquito population and prevent malaria transmission,” the CAO said.
Additionally, he urged the government and all stakeholders to prioritize the upgrading of the different health centers, particularly Akokoro and Teboke Health Centers, from Health Center III to Health Center IV, citing that this move will improve service delivery and ensure that people have access to the quality healthcare they deserve.
Apac district LC5 chairperson, Odongo Asanti is seemingly hopeful that with the launch of this malaria vaccine, the government is now taking a decisive step toward defeating malaria in Apac and across Uganda.
Odongo noted that malaria has long been a thorn in Apac, affecting several communities socially and economically.
“Malaria has contributed to school dropouts, poor academic performance, poverty, and even domestic violence. In some instances, malaria-related deaths in our district have been linked to witchcraft due to the high levels of misconception surrounding the disease,” Odongo said.
Furthermore, he appealed to the government for additional funding for road rehabilitation, especially for roads like Apoi, Akokoro, and Alengakur, urging that these particular roads are crucial for improving accessibility to health facilities, which will be essential in ensuring that people can receive timely care and vaccination.
Dr. Daniel Odongo, the District Health Officer for Apac, emphasized the importance of the vaccine in addressing the district’s persistent malaria problem.
“In Apac district, malaria continues to be the leading cause of illness and death. Apac is in category one! This vaccination campaign is an essential tool in our fight to reduce the disease burden and improve the overall health of our children,” Dr. Odongo said.
Apac district woman MP Betty Aworo Engola extended her heartfelt gratitude to the government for allocating shs673 million to support the construction of a modern medical store at Apac Hospital.
“This is an important step in ensuring we have the necessary infrastructure to support our health system,” she added.
She also called for the relocation of the malaria control program to Lango sub-region, noting that Lango has been a malaria hotspot for many years.
The woman MP proposed that the government establish an institute at Lira University to focus on malaria research, particularly on new drugs and methods for testing and controlling the spread of malaria.
“As we strengthen our fight against malaria, it is also essential that we support our health workers, particularly those who have formed a savings and credit cooperative (SACCO) in 2023. The government must assist these health workers in their efforts to improve their livelihood,” said Mrs. Engola.
“Lastly, our health facilities need proper infrastructure to function effectively. I urge the government to prioritize the provision of a police patrol vehicle for our health facilities and ensure that power connectivity is extended to all health centers. The rehabilitation of our road network is also vital to improve access to healthcare.”
Patrick Ocan, Member of Parliament for Apac municipality, expressed his support for the vaccination program.
“This is a historic moment for Uganda, and it is one that will save many lives. We encourage all parents to ensure their children are vaccinated, as this will help build a malaria-free future for our children and communities,” Ocan said.
MP Engola had to agree with MP Ocan, stating, “As a mother and a representative of the people, I am thrilled with this new development. It is a game-changer that will protect our children and contribute to a healthier Uganda.”
Meanwhile, Dr. Robin Nandy, the UNICEF Representative in Uganda, emphasized the need for continued efforts to complement vaccination with other malaria prevention measures, including the use of insecticide-treated nets, indoor residual spraying, and seasonal malaria chemoprevention.
“The malaria vaccine is an important addition to Uganda’s malaria control efforts, but it must work in tandem with other proven prevention strategies to ensure lasting impact,” Dr. Nandy stated.
WHO Representative to Uganda, Dr. Kasonde Mwinga, hailed the launch, noting that Uganda is the 19th African country to integrate the malaria vaccine into its routine immunization program.
“By integrating the malaria vaccine into routine immunization, Uganda is taking a bold step to protect its children, save lives, and secure a healthier future,” said Dr. Mwinga.
Dr. Charles Olaro, Director General of Health Services emphasized the importance of ensuring that every child under 18 months receives the R21/Matrix-M malaria vaccine, as outlined in our national immunization schedule.
“This vaccine is crucial in the fight against malaria, and we need to make sure it reaches every child in Uganda,” he said.
“To all our dedicated health workers, I urge you to administer this vaccine with the utmost dedication and commitment. Your role is vital in saving lives and protecting the future of our children,” Dr. Olaro added.
He also encouraged leaders to help dispel any negativity or misconceptions surrounding this vaccine. “Public trust is key to the success of any vaccination program, and we all have a responsibility to ensure that our communities understand the importance of this vaccine in eliminating malaria.”
Testimonials from beneficiaries
Mothers whose children have benefited from the malaria vaccine shared their gratitude for the life-saving intervention.
Annet Atim expressed relief, saying, “I am happy that my child has received the malaria vaccine. Malaria has caused us so much pain in the past, but I am now confident that my child is protected.”
Another mother, Dinah Atim, from a rural village in Apac, spoke about the peace of mind the vaccine has given her. “Malaria has always been a constant threat to our children, and I almost lost a child before due to severe malaria. This vaccine is a blessing to all mothers in our community.”
Hellen Akullu, a mother from a neighboring village, not far off from the launch venue, shared her excitement about the vaccine’s role in safeguarding her children.
“I encourage all mothers to bring their children for the malaria vaccine. We cannot afford to lose any more children to malaria.”
Uganda and the rest
The country has set an ambitious goal to eliminate malaria by 2030, and this new vaccination program is expected to be a game-changer in achieving that target.
Uganda joins other African nations taking bold steps to combat malaria, while the global partners are working tirelessly to ensure the success of the vaccination campaign.
Parents, caregivers, and communities are encouraged to seize this life-saving opportunity and safeguard future generations’ health.
Discover more from tndNews, Uganda
Subscribe to get the latest posts sent to your email.